![]() 5 minute read
5 minute read
The matter of Public Health has always been the challenging one and different across the globe. The urban architecture plays the critical role for citizens health. At the same time, Estonia starts a new nation broad genetic profiling, personalized medication enters the market, and aging is considered a disease. Can those innovative approaches turn against human health by overdiagnosing?
City Health
Is the Public Health issue a nationwide challenge, local problem, or personal responsibility? The term itself was invented in the 19th century with a raising need for city sanitation. The impact of urban planning on various life and economic aspects is undeniable. According to the Healthy Cities Consensus by World Health Organization in Shanghai in 2016: “Health is created at the local level, in the settings of everyday life.” The car-dominated transportation system, reduced opportunities for physical activity, and lack of social connection all impact on public health. The lifestyle is changing towards less physically active. The percentage of obese people in Holland will increase from 49 percent in 2009 up to 62 percent in 2040. With the major urbanization trend, the potential mega-cities have to think of their design already today to support the health in their areas.
Outdoor urban air pollution kills some 1.2 million people worldwide. In addition, road injuries are the leading cause of death for young adults. City planning can ensure the basic safety as well as nudge citizens towards more active lifestyle. For instance, the cycling cities like Copenhagen and Amsterdam have a great benefit for its habitats. Studies have shown that cycling commuters live longer reducing the risk of dying from cardiovascular conditions by 52%. Another research, “Physical activity in relation to urban environments in 14 cities worldwide” says: “Design of urban environments has the potential to contribute substantially to physical activity. The similarity of findings across cities suggests the promise of engaging urban planning, transportation, and parks sectors in efforts to reduce the health burden of the global physical inactivity pandemic.”
Nationwide
DNA testing
While Smart Urban planning is one of the ways to enhance cities health conditions, the DNA testing and proper medical recommendations can help to prevent chronical illnesses. Estonia offers to its residents free genetic testing to develop personalized medicine in national health care. National Personalized Medicine programme gathers 100,000 new biobank participants. Family doctors will receive the genetic citizens’ genetic information and deliver to patients counseling about the results and recommendation to their lifestyle. Eventually, the program is planned to expand offering free DNA testing for the whole population.
“Today we have enough knowledge about both the genetic risk of complex diseases and the interindividual variability of the effects of medicines in order to start using this information systematically in everyday healthcare,” said Jevgeni Ossinovski, Minister of Health and Labour. ” In cooperation with the National Institute for Health Development and the University of Tartu, we will enable another 100,000 people to join the Estonian biobank, to boost the development of personalized medicine in Estonia and thus contribute to the advancement of preventive healthcare.” The ethical part of the study has been addressed as well. The genetic data entirely belongs to a donor, and he or she can choose which research programs can use the data.
The genetic testing program has previously been offered in the UK by NHS. Nonetheless, the testing had a fee and helped doctors to diagnose the diseases not to prevent them. At the moment, there are half a million DNA entries with the personal characteristics to U.K. Biobank. Participants of the study are being followed with years to come. The technological development only benefits the research. The Global Biobank and the collaborations on research subject can open new reality of the public health.
Price of ageing
By 2050, the world’s population aged 60 and over will exceed 2 billion which is tripled from 2000. Most of this increase is occurring in less developed countries, where the elderly population will reach 1.7 billion. While all nations can benefit from the extended life expectancy, it will depend on the public health policies and the quality of the services.
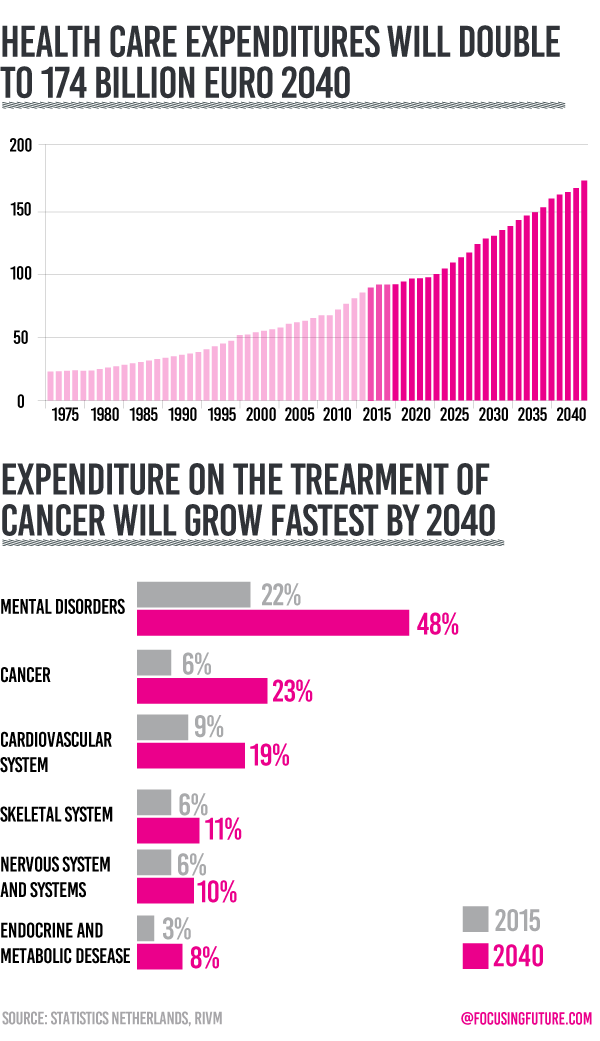
According to Public Health Foresight study, Dutch Health care expenditures will double to 174 billion euro in 2040 reaching 9,600 euro per capita from 5,100 euro in 2015. Yearly increase by 2040 would be 2.9 percent on average. One-third of the costs would be attributed to the ageing of the population and population growth. The group with the highest spending rates will remain mental disorders like dementia and intellectual disabilities. A significant increase would be caused by treatment of cancer and cardiovascular diseases.
Japan, the country with the oldest and fast-ageing population, is struggling with increasing welfare spending.The Ministry of Health, Labor, and Welfare announced investments towards medical research in precision and personalized medicine. The government increases spending to $4.6 billion for 2018 while the cost of ageing citizens is estimated to reach $5 billion. The research is expected to deepen the understanding and develop treatments for chronic diseases. Evidently, the prevention of symptoms related to the age and genetical predisposition is one of the strategies of Japan.
As Prime Minister Abe comments: “Amidst the rapid approach of the year 2025, when all the baby boomers will have reached 75 years of age, technologies of the fourth industrial revolution will play an important role in improving our social security system, including the responses to the issues related to dementia.” At the same time, the government is seeking to provide universal health care coverage. The goal is to ensure basic health services to 1 billion more people by 2023.